Adult Snoring
Snoring is a problem for a lot of adults, or more specifically for their partner! Snoring is generally created by turbulent (disturbed) airflow when the airway passage from the teeth to the windpipe is narrow and / or floppy.
The commonest causes for a narrow airway include:
Nose Blockage
From deviated septum, turbinate swelling, hayfever, sinusitis.
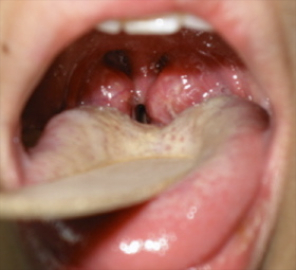
Throat Blockage
Large tongue, large tonsils, long floppy palate
Neck Blockage
Excessive weight in the neck, narrowing the internally breathing passage and placing excessive pressure on the airway tissues. The neck blockage is usually associated with being generally overweight.
More on adult snoring
Snoring is a problem for a lot of adults, or more specifically for their partner! Snoring is generally created by turbulent (disturbed) airflow when the airway passage from the teeth to the windpipe is narrow and/ or floppy.
The problems caused by benign (or simple) snoring are largely social and affect mostly the partner.
Sleepless nights for the partner are initially amusing to the snorer, but may become serious eventually threatening the relationship.
Snoring may also be associated with Obstructive Sleep Apnoea (OSA), which is defined as a period where the adult snoring patient actually stops breathing (usually for more than 10 seconds) due to the blockage in the airway.
OSA may have very serious long term consequences on health.
Videos relating to Adult Snoring
Additional information
All causes of death
Patients with severe OSA have a 3 to 6 fold increase in all causes of mortality compared to patients without OSA.
Heart disease
Increased risk of blood pressure, lung blood pressure (pulmonary hypertension), abnormal heart rhythms, heart attacks and heart failure. The heart risks are largely related to the increased stress on the heart from pumping against higher pressures in the chest.
Stroke (brain attack)
Increased risk of stroke especially in severe OSA.
Day Time Function (brain performance)
Increased morning headaches, daytime sleepiness, fatigue, inattention, poor memory, increased likelihood of mistakes during work and recreation performance.
Mental Illness
Has been demonstrated to be associated with increased depression.
Car Accidents
Much higher incidence of motor vehicle accident and death with OSA patients.
Good Sleep hygiene
Appropriate environment, no electronic devices, regular sleep schedule, avoid alcohol and smoking
Weight Loss
Pressure Machine
The Continuous Positive Airway Pressure (CPAP) device is the gold standard for treating OSA. The machine has a mask that fits over the face, connected via a tube to a machine, that continuously pumps positive pressure air into the airway of the sleeping patient, preventing collapse of the tissues.
Dental Splint Device
Since a large tongue can contribute to blockage and the tongue attaches to the jaw, dental splint devices work on the fact that moving the jaw forward will move the tongue forward. This is an effective treatment method in appropriately selected patients.
ENT Surgery
Surgery to unblock either the nose or the throat or both maybe suggested to improve CPAP mask use; or in an attempt to treat OSA without the CPAP mask. Nasal surgery most commonly involves straightening the septum (Septoplasty) and reducing turbinate size (turbinate reduction or turbinoplasty). Throat surgery most commonly involves tonsillectomy (+/- palate surgery called palatoplasty). Your ENT Surgeon (otolaryngologist) will make recommendations on surgery, if appropriate.
Patients who snore and are concerned about their symptoms should be evaluated by an ENT (Otolaryngologist) Surgeon to assess their airway for blockage points. A test for sleep apnea diagnosis is then usually suggested, this is called a sleep study (Polysomnogram).
Other Services
Other Services
Still have a question?
Our team will be happy to answer any questions you may have about Adult Snoring.
More About Tonsils, Adenoids, and Tonsilitis
Tonsillitis refers to inflammation of the pharyngeal tonsils. The inflammation may involve other areas of the back of the throat including the tonsils and adenoids and the lingual tonsils (areas of tonsil tissue at the back of the tongue). There are several variations of tonsillitis: acute, recurrent, and chronic tonsillitis and peritonsillar abscess.
The type of tonsillitis determines what symptoms will occur:
Acute tonsillitis
Patients have a fever, sore throat, foul breath, dysphagia (difficulty swallowing), odynophagia (painful swallowing), and tender cervical lymph nodes.
Recurrent tonsillitis
This diagnosis is made when an individual has multiple episodes of acute tonsillitis in a year.
Chronic tonsillitis
Individuals often have chronic sore throat, bad breath, tonsillitis, and persistently tender cervical nodes.
Peritonsillar abscess
Individuals often have severe throat pain, fever, drooling, foul breath, trismus (difficulty opening the mouth), and muffled voice quality, such as the “hot potato” voice.
Tonsillitis is usually treated with a regimen of antibiotics. Fluid replacement and pain control are important. Hospitalisation may be required in severe cases, particularly when there is airway obstruction.
When the condition is chronic or recurrent, a surgical procedure to remove the tonsils, tonsillectomy, is often recommended.
For some patients, a surgical procedure to remove the tonsils (and adenoids if they cause health issues) is required, which requires a stay in hospital. The tonsillectomy or adenotonsillectomy surgery is minimally invasive, performed through the throat and with cameras through the nose, and requires a general anaesthetic.
An overnight stay in hospital is required if your child is under 4 years of age. If your child is over the age of 4 then often the procedure can be performed as a day surgery procedure. Here is a link to a quick children’s video
A variety of tools may be used to remove the tonsils and/or adenoids, including harmonic scalpel, plasma dissection, cold dissection, laser and electrocautery. Your surgeon will decide which is the best option for your particular case.
Many patients require around 2 weeks off either school or work to recover from the surgery, with post-operative pain the most concerning symptom.