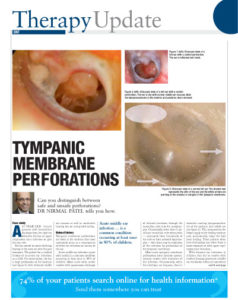
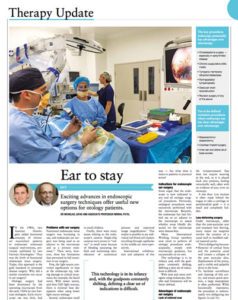
Holes in Eardrum
Holes in eardrum and the anatomy of the ear
In order to understand chronic ear infection and holes in eardrum are caused, one must have some knowledge of the hearing mechanism.
Anatomy of the Outer Ear
The auricle and the external ear canal make up the outer ear. Here, the sound waves are collected and amplified, to be transmitted to the eardrum.
Anatomy of the Middle Ear
The section behind the eardrum and before the inner ear is the middle ear, home to the three hearing bones (the hammer, anvil and stirrup). Vibrations from the sound waves collected by the outer ear are collected, and transmitted to the fluid-filled space of the inner ear by the three bones. Lining the middle ear chamber is a membrane similar to your nasal lining. The membrane contains blood vessels and mucous glands, and is punctuated by the Eustachian tube, which connects the middle ear to the back of the nose.
The Eustachian tube is needed to equalise pressure in the middle ear when differentials occur. Opening your Eustachian tube during a plane flight or other altitude change results in a ‘popping’ sensation and reduction of pressure inside your ear.
Anatomy of the Inner Ear
The chamber behind a dense layer of bone is the inner ear. It is lined with a delicate membrane and filled with fluid, which transfers the vibration of the stirrup bone into fluid waves, which are transformed into electrical impulses by hair cells in the cochlea.
Video by Associate Professor Nirmal Patel.
Additional information
If the eardrum and three small ear bones become chronically infected, perforations in the ear drum and/or destruction of the small ear bones can result. Scar tissue formation can also cause hearing problems. Any of these conditions can create conductive hearing loss.
Conductive hearing loss occurs when something interferes with the transmission of sound waves from the outside world to the cochlea. In chronic ear disease, the scar tissue may block the sound waves, or destruction of the ear bones or perforations of the ear drum may prevent effective transmission.
Less frequently, cholesteatoma (growth of eardrum skin in the middle ear chamber) can result from chronic ear disease. Cholesteatoma is treated surgically – the misplaced tissue is removed to prevent serious complications such as deafness, facial weakness, permanent dizziness and abscesses in the brain.
If ear drainage is the main concern, the medical treatment option is taken. Careful cleaning of the ear, topical antibiotics (in the form of Ciprofloxacin antibiotic drops) and sometimes oral antibiotics are used to control the infection and therefore the drainage.
Surgery has been the recommended option for chronic ear disease for decades,since the use of the operating microscope became commonplace. It is necessary to eliminate the bacterial colonisation and therefore prevent serious complications. However, surgery can now reconstruct the part of the hearing mechanism which is causing problems, also.
Prosthetic ear bones made of plastic can replace any diseased ear bones in the middle ear; alternatively cartilage may be used or the bone may be relocated. Tissue grafts made of a layer of muscle and a layer of cartilage are used to repair the perforation in the eardrum.
To prevent the formation of scar tissue and help normalise middle ear function, a thin plastic sheet is often inserted behind the eardrum. If the chronic ear disease has progressed to fill the ear with scar tissue, or if the ear bones have been completely destroyed, surgeons will perform the operation in two stages. At first, the plastic sheet will be inserted to allow normal healing without scar tissue formation. In the next operation, the plastic sheet is removed and prosthetic ear bones will be placed to attempt to restore hearing. It won’t be known until the time of your first surgery whether it will be necessary to separate the two stages of the operation.
If a permanent perforation in the eardrum remains after the ear infection subsides, a myringoplasty may be required to close up the hole. Myringoplasties are performed when there is no residual infection, and the ear bones of the middle ear are healthy. When the middle ear is sealed, an improvement in hearing is usually apparent.
Myringoplasty can be performed either through the ear canal or via an incision behind the ear. Operations performed through the ear canal can be done under local anaesthetic, whereas posterior incision operations are dozen under general anaesthetic. The surgeons use your own ear tissue to repair the hole in the eardrum, which should be fully healed in around 3 months. When healing is complete, you should notice a concurrent improvement in hearing.
If your ear infection has resulted in eardrum perforation or damage to any of the mucosa or ear bones, tympanoplasty may be performed to repair the structures and clear up any residual infection. The tympanoplasty will close the perforation of the ear drum, and repair damage to the structures that transmit sound. Hearing is almost immediately improved in many cases, and if eardrum repair is not required, the operation may be performed through the ear canal with no incision, on an outpatient basis.
Generally, though, tympanoplasty is performed through an incision behind the ear, and requires general anaesthesia. Tissue from the chewing muscle is harvested to repair the perforation of the eardrum, and if the ear bones have become diseased, they may be replaced with artificial prosthetic ear bones. These prostheses can remain in your ear and functional for the rest of your life.
Some patients may need more than one operation to repair both the ear bones and the ear drum. If this is the case, the ear drum is repaired first. Once this is fully healed in around 6 months, the prosthetic sound transmitting mechanisms can be inserted.
Unless there are unusual complications, an overnight stay in hospital should not be required. Patients can return to work within around four to six days; however, improvement in hearing may not come for some time after the surgery due to the healing process. You can expect a noticeable improvement in hearing within 3 months.
Some symptoms are common to all ear operations, including:
Dry Mouth and Taste Disturbances
Your mouth may feel dry and taste may be disturbed for several weeks after the device is implanted.
Loss of Surface Sensation
You may lose surface sensation on your outer ear following cochlear implant surgery, in small areas or across the entire ear. This usually resolves spontaneously within 6 months after surgery.
Tinnitus
Tinnitus does not usually improve immediately after surgery, but usually decreases in proportion to the hearing improvement obtained. If the hearing remains unimproved following surgery for chronic ear disease, the tinnitus will remain or sometimes worsen.
Pain and Stiffness of the Ear and Jaw
Pain and stiffness in the ear and jaw are common following surgeries for chronic ear disease. Ear pain and jaw pain can worsen when you chew or move your neck, and will persist for at least 7 days after the surgery. It can be controlled with pain killers, and any remaining stiffness should subside within 4 to 8 weeks.
As the ear heals, itching is common. As nerve fibres regrow into the new tissue, occasional sharp shooting pains are common.
Other Services
Other Services
Still have a question?
Our team will be happy to answer any questions you may have about Holes in Eardrum.